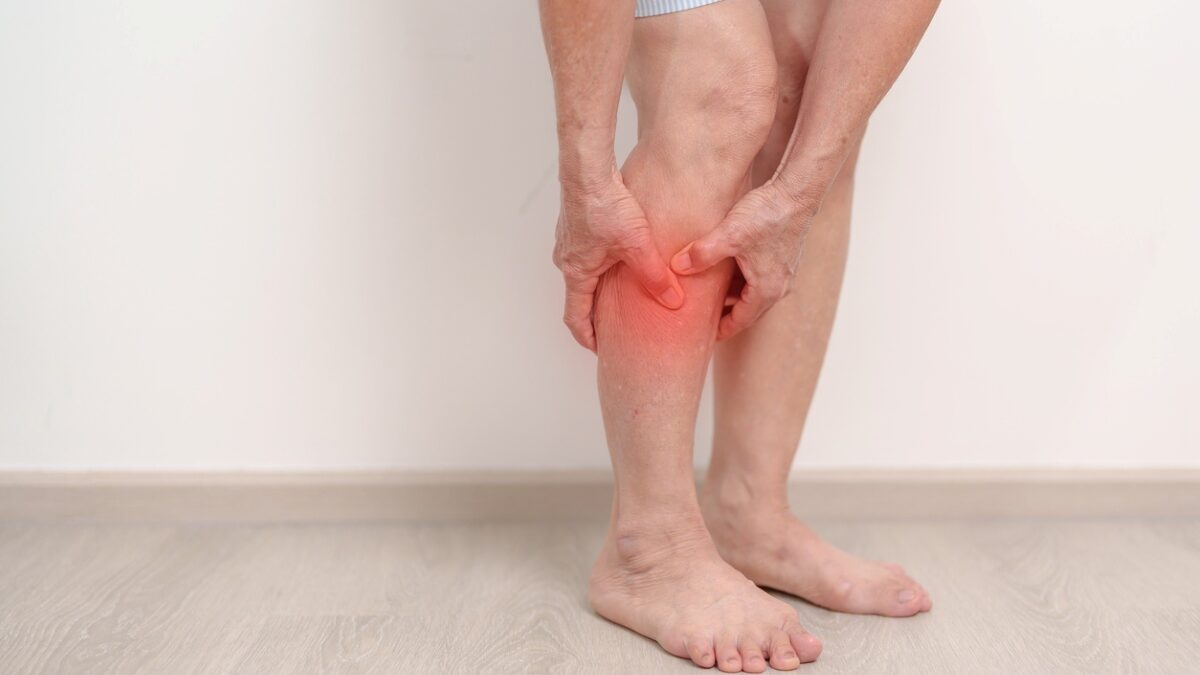
Deep vein thrombosis, or DVT, is a blood clot that forms in a deep vein, usually in the lower leg or thigh. These clots develop when blood flow slows down, the blood becomes more prone to clotting, or the walls of a blood vessel become injured or irritated. While a DVT on its own is a serious medical concern, the bigger danger is what happens if part of that clot breaks free and travels to the lungs. This is called a pulmonary embolism, or PE. A PE can block blood flow in the lungs, put intense strain on the heart, and become life-threatening quickly.
Knowing the warning signs of DVT and PE, understanding your personal risk factors, and recognizing when to seek emergency care can be lifesaving.
How to Tell if You Have DVT
Most people with a DVT notice symptoms on one side of the body, not both. You might see swelling in one foot, ankle, calf, or thigh but not the other. The affected leg may feel sore, warm to the touch, or tight in a way that doesn’t match any recent activity. Some people also notice redness or changes in skin color over the area, along with a feeling of heaviness in the leg.
A helpful way to think about it: if you wake up and one leg looks noticeably bigger than the other, or your calf hurts when you walk and you can’t explain why, it is worth getting checked. DVT is not the most common cause of leg pain, but it is one of the most important to rule out.
When a Clot Travels to the Lungs
A pulmonary embolism happens when a blood clot blocks an artery in the lungs. This reduces the body’s ability to exchange oxygen and puts serious strain on the heart. Some PEs are small, but others can cause sudden collapse. PE symptoms can also mimic other conditions like anxiety, asthma, or heart problems, which is why it is important to act fast when the pattern fits.
PE symptoms often happen suddenly and feel out of proportion to what you were doing. You might feel short of breath while sitting still, or have sharp chest pain that gets worse when you take a deep breath or cough. Other warning signs include a rapid or pounding heartbeat, feeling faint or dizzy, coughing up blood, or new and unexplained anxiety paired with breathing problems.
If you experience any combination of these symptoms, especially alongside leg swelling or known risk factors for clots, call 911 or get to an emergency room immediately. A PE is not a situation where you should wait out your symptoms at home.
Who Is at Higher Risk for Blood Clots?
Anyone can develop a blood clot, but certain situations raise the risk more than most people realize. Many people are surprised to learn that everyday scenarios like long travel or a recent illness can increase clot risk significantly.
Recent surgery is one of the biggest risk factors, especially orthopedic procedures or major abdominal surgery. Long periods of immobility, whether from bed rest, a long car ride, or a cross-country flight, also slow blood flow enough to make clots more likely.
Pregnancy and the postpartum period change how the blood clots, which raises the risk. Hormone therapy and certain birth control methods can have a similar effect, particularly when combined with smoking. A personal or family history of blood clots, cancer and some cancer treatments, obesity, smoking, severe dehydration, and certain inherited clotting disorders all add to the risk.
Multiple risk factors can also combine to increase risk. Someone who recently had surgery and then sits on a long flight faces a higher combined risk than either situation alone.
DVT or Pulled Muscle? How to Tell the Difference
This is one of the most common questions, and for good reason. A pulled calf muscle can feel a lot like a blood clot. Both cause soreness, tightness, and discomfort when you walk.
A muscle strain usually follows a clear event like exercise or an awkward step. The pain tends to get worse with specific movements and then improves with rest over a few days. A DVT is more likely when the swelling is only on one side, the leg feels warm, and the pain doesn’t match the level of activity you’ve done. If you also have risk factors like recent travel, surgery, pregnancy, or a prior clot, a medical evaluation is a good idea even if the symptoms seem mild.
Lowering Your Risk in Everyday Life
You can’t prevent every blood clot, but there are practical steps you can take during common high-risk situations like travel, recovery from surgery, or periods of illness or injury.
Move your legs regularly during long travel, and take breaks to walk when you can. Stay hydrated, especially when flying or when you are sick. Follow your post-surgery instructions carefully, including any mobility recommendations from your care team.
If you have major risk factors or a history of blood clots, ask your doctor about whether additional clot prevention measures make sense for you. If you are already taking blood-thinning medication, take it exactly as prescribed and do not skip doses without medical guidance.
Know When to Seek Help for Leg Swelling
Not every swollen leg needs emergency care. But there are situations where getting checked quickly can be lifesaving. You should seek urgent evaluation if one leg swells suddenly or keeps getting worse, especially if accompanied by warmth, redness, or calf pain. A history of blood clots or major risk factors is another reason to take symptoms seriously.
The most important red flag is when leg symptoms show up alongside chest symptoms. If you have a swollen leg and you suddenly become short of breath, develop chest pain, feel faint, or cough up blood, treat it as an emergency right away.
Your Next Step If Something Feels Off
Blood clots are treatable, but they are time-sensitive. A swollen leg could turn out to be something simple, but if it is a DVT, early evaluation gives you the best chance of preventing a pulmonary embolism. Fast evaluation also means more treatment options and fewer complications. With access to on-site lab and imaging services, an ER can quickly confirm or rule out a clot.
Life Savers ER is open 24/7 with no wait times. If you are experiencing leg swelling, calf pain, chest pain, or shortness of breath, don’t wait to see if it passes. Walk in to one of our locations for immediate emergency care.